March 13, 2026
The Final Journey is not always Peaceful
The final journey is not always peaceful: Why euthanasia is less well researched medically than life-saving treatments by science writer, Manuela Callari in Medscape (German).
Everything had been prepared down to the last detail for a final, peaceful farewell.
Family and friends had gathered, and a pianist played softly in the background. In this highly emotional atmosphere, Arjen Göbel, a GP in Amstelveen, the Netherlands, began the procedure intended to bring his patient’s life to a planned and peaceful end. But things turned out differently than expected.
A farewell that gets out of hand
Following the standard protocol in the Netherlands, he first injected a drug to render her unconscious. The 48-year-old breast cancer patient closed her eyes; her breathing became shallower. Yet death did not come. The patient continued to breathe – and her relatives noticed it, as did the doctor, who remained outwardly calm.
Then suddenly her voice broke the silence. From her bed, she opened her eyes, looked directly at the doctor and asked in Dutch: “Gebeurt er nog wat of hoe zit dat?” – “Is something else going to happen, or what’s going on now?”
Göbel felt a wave of panic wash over him. The carefully planned moment of peace had turned into an absurd nightmare. He ran to his car, fetched a spare kit and repeated the procedure. But the patient remained awake and responsive.
Finally, Göbel called the ambulance service whilst he fetched two more emergency kits from a nearby pharmacy. Together with the paramedics, he injected the lethal mixture of drugs directly into a vein in the groin area – to no effect.
Only after a further injection, this time into the carotid artery, did death occur.
It was now 6 pm, four and a half hours after the first injection. What had been intended as a dignified farewell had turned into a long, traumatic ordeal. “It was the worst thing I have ever experienced,” Göbel later told Medscape.
In principle, every procedure carries risks: our bodies do not always react predictably, and complications can arise even during routine procedures.
In virtually all other areas of medicine, interventions are underpinned by extensive clinical trials, precise dosage studies and strict regulatory procedures.
In the case of euthanasia and assisted dying, this safety net is largely absent.
Despite the far-reaching nature of the act, the pharmacology is astonishingly poorly substantiated scientifically – there is hardly any reliable data.

A range of bottles of liquid Nembutal from South America
What is euthanasia, and what is assisted dying?
Euthanasia refers to the deliberate, direct administration of a lethal drug by a doctor to end a patient’s life at their express request. A prerequisite is usually the presence of suffering deemed unbearable.
Assisted dying, on the other hand, refers to a procedure in which lethal drugs are prescribed by a doctor, but are taken voluntarily and independently by the person concerned.
The crucial difference is that it is not the doctor, but the patient themselves who takes the final, fatal step.
Patients wish for a peaceful, pain-free death
The issue is polarising: across Europe, countries are grappling with the ethical question of whether and how patients may be assisted in dying.
The aim is almost always a peaceful, pain-free death. But are doctors actually able to fulfil this promise? A look at current practice raises doubts.
In many places, there is a lack of clear regulations, binding standards and uniform controls. Instead, a patchwork of differing procedures and laws has emerged across the continent, based less on transparent scientific evidence than on trust and assumptions.
This raises a fundamental question: do people who wish to exercise their final act of self-determination and consciously end their lives not deserve the same clinical care, the same safety standards and the same scientific evidence as those whose treatment aims to prolong life?
A long road to legalisation, even in the Netherlands
Internationally, the Netherlands is regarded as a kind of gold standard for end-of-life regulations.
In 2002, the government became the first in the world to legalise euthanasia.
In doing so, it enshrined in law a practice that had previously been tolerated for decades. Yet even here, a closer look reveals that the scientific basis for the procedures used has developed in a surprisingly informal manner.
The public debate was triggered in the early 1970s by a single case that caused quite a stir.
In 1971, Geertruida Postma, a GP in the North Frisian village of Noordwolde, helped her mother to die.
She injected 200 mg of morphine directly into a vein.
Her mother was 79 years old, lived in a care home, was partially paralysed following a brain haemorrhage, deaf, suffering from severe pneumonia, barely able to speak, and had already attempted suicide once.
Her death would probably not have attracted any attention.
But Postma informed the care home management. They spoke to the health authorities.
The result: a charge carrying a theoretical maximum sentence of 12 years’ imprisonment.
When Postma stood trial in 1973, the mood shifted.
Numerous doctors admitted in an open letter to the Minister of Justice that they had done similar things themselves.
Around 2,000 people from Postma’s home town signed a declaration in support of euthanasia. Patients founded the Nederlandse Vereniging voor een Vrijwillig Levenseinde (NVVE), which gained more than 1,000 members within a few days and now has over 177,000.
Although the court found Postma guilty, it imposed only a suspended sentence.
This symbolic verdict reflected broad social acceptance, as Bert Keizer, a former geriatrician from Amsterdam, later explained to Medscape.
From an isolated case to a standardised protocol
Nevertheless, there remained considerable reluctance within the medical profession.
Many doctors continued to find euthanasia frightening and actually wanted nothing to do with it, according to Annemieke Horikx of the Royal Dutch Pharmacists Association (KNMP).
In order to at least standardise the choice of medication, the KNMP developed a standardised protocol for the first time in 1987.
However, genuine interprofessional collaboration came surprisingly late. It was not until around 2010 – eight years after the law on ending life on request came into force – that doctors began to systematically seek dialogue with pharmacists.
This resulted in the first joint protocol in 2012, which was last substantially updated in 2021.
Today, the Dutch standard is based on a two-stage intravenous procedure.
First, a high dose of anaesthetic is administered, usually propofol, to induce a deep coma.
This is followed by a muscle relaxant such as rocuronium, which paralyses the respiratory muscles.
A small dose of lidocaine is often injected beforehand to alleviate the burning sensation caused by the anaesthetic.
Despite this standardisation, it is clear that even in a pioneering country, the procedure is the result less of traditional clinical research than of a decades-long, socially negotiated learning process.
Thiopental is no longer available
For many years, thiopental was regarded as the reliable standard for inducing a coma in euthanasia: fast-acting and predictable.
However, following the EU-wide export ban on drugs that could be used in executions, the active ingredient began to disappear from the market from 2011 onwards.
Manufacturers withdrew, supplies were strictly controlled – thiopental is now scarcely available.
In response, the Netherlands adapted its guidelines.
Doctors switched to propofol, an effective but less than ideal substitute that must be administered in significantly higher doses to achieve a sufficiently deep coma.
A bottle of Nembutal, as used at DignitasThe protocols are being further developed
Since the introduction of the first Dutch standards in 1987, the active substances used have remained largely unchanged at their core.
The guidelines themselves, however, have undergone a fundamental transformation: what were once comparatively simple drug recommendations have become detailed, process-oriented instructions.
The latest comprehensive update from 2021 marks an important step towards greater formalisation.
There is now a particular focus on so-called ‘exceptional situations’, i.e. cases in which patients do not lose consciousness sufficiently despite the procedure being carried out according to the rules, or death does not occur as expected.
The guideline now contains precise guidelines for the management of difficult vascular conditions, such as those frequently encountered in oncology patients. These are supplemented by specific recommendations for flushing venous access points with sodium chloride between individual injections to prevent drug precipitation.
Furthermore, standardised tests of the corneal reflex are required to ensure the presence of a deep coma prior to the administration of the neuromuscular blocker.
Although around 97% of those affected opt for intravenous administration, Dutch law also permits assisted dying as distinct from euthanasia.
In this case, the lethal medication is not administered by medical staff, but by the patient themselves.
Oral doses of pentobarbital or secobarbital are used, which exceed therapeutic doses many times over. The preparations are often flavoured to mask the intensely bitter taste.
In addition, experts recommend the prophylactic administration of antiemetics, as nausea and vomiting are known side effects.
As Annemieke Horikx explains, the oral method is less easily controlled pharmacologically and clinically: ingesting around 100 ml of a strongly bitter solution can lead to vomiting, and the onset of unconsciousness and death is more variable and, in some cases, significantly delayed.
Nevertheless, in the majority of cases, death occurs within about 30 minutes.
The oral route can take several hours and is associated with higher risks, confirmed Steven Pleiter, former director of the Dutch Centre of Expertise on Euthanasia.
If patients vomit the bitter mixture, only a partial amount may be absorbed. This can lead to a prolonged, confused state without death occurring.
In the Netherlands, a doctor is legally authorised in such a case to intervene and administer a lethal injection.
In countries where only assisted dying, but not euthanasia, is permitted – such as Switzerland and Austria – no such safety net exists.
In Italy, moreover, the pharmacological procedure is not a nationally established standard as it is in the Netherlands.
Instead, a doctor is appointed for each individual case to determine a personalised medication regimen and administration procedure, which is subsequently reviewed and approved by a clinical committee.
A regulatory vacuum
The examples show that countries are developing their own, sometimes differing protocols. There is virtually no valid data.
By way of comparison: if a pharmaceutical company wishes to bring a new drug to market – be it for the treatment of a skin condition or a specific form of cancer – it must undergo years of clinical trials in phases 1, 2 and 3.
Safety, efficacy and dosage profiles must be demonstrated to the European Medicines Agency (EMA).
However, no comparable regulatory framework appears to exist for medicines used to end a person’s life.
“The medicines used in assisted dying or euthanasia are not authorised for a lethal purpose,” a spokesperson for the EMA wrote to Medscape. The agency regards this as a matter of national jurisdiction.
What is the stance of national authorities in Europe?
The Dutch Medicines Act permits the prescription of medicines outside their authorised indications, provided that protocols or standards have been developed within the relevant professional association.
If these are still being developed, consultation between the treating doctor and the pharmacy is mandatory.
The Federal Institute for Drugs and Medical Devices (BfArM) informed Medscape that, following a court ruling, it was “no longer dealing with this issue”.
The Italian Medicines Agency, Agenzia Italiana del Farmaco (AIFA), made similar comments. There is no official national standard for medication used in medically assisted dying.
Instead, arrangements are made on a case-by-case basis under the supervision of local health authorities and ethics committees – based on a 2019 ruling by the Constitutional Court.
Euthanasia and assisted dying in the European Union
In the United Kingdom, where the Terminally Ill Adults (End of Life) Bill is currently being debated in the House of Lords, a clearer regulatory path is emerging.
A spokesperson for the Medicines and Healthcare Products Regulatory Agency told Medscape that, should the Bill receive Royal Assent, the responsible minister would develop a regulatory process to define authorised substances and regulate their provision and monitoring.
Currently, medicines used for the purposes of euthanasia or assisted dying are used off-label.
Doctors use anaesthetics and muscle relaxants approved for surgical procedures in doses significantly exceeding the therapeutic limit – for a purpose, namely death, for which they were never approved.
In the Netherlands, supervision is strict but is fundamentally retrospective in nature and focused on assessing legal compliance, not clinical outcomes.
Once the procedure is complete and the patient has died, the attending doctor informs the local coroner, who investigates the death and notifies one of the five regional euthanasia review committees (RTE).
Each of these consists of a lawyer, a doctor and an ethicist.
According to the latest RTE report from 2024, 9,958 reports were received that year.
In six cases, the commissions concluded that the doctor had not complied with the ‘due care criteria’.
In three cases, there was a risk that the patient experienced the effects of the muscle relaxant whilst conscious.
In two cases, no independent medical consultation had taken place.
In another case, the doctor had failed to exercise the necessary “special caution” by not seeking psychiatric expertise in response to a request for assisted dying that was predominantly based on psychiatric grounds.
Extensive preparation
“We check whether the doctor has complied with the due diligence criteria,” says Keizer.
“Was the suffering unbearable?
Was the request voluntary?
We do not analyse the deceased’s blood to check whether the drug levels were correct.”
As long as no gross technical error is reported – such as the patient waking up again – the physiological details of the dying process are not investigated further, according to Keizer.
Due diligence criteria in the Netherlands
The due diligence criteria of the Dutch Act on Termination of Life on Request and Assisted Suicide stipulate that the doctor:
- must be convinced that the patient’s request is voluntary and well-considered,
- must be convinced that the suffering is unbearable and there is no prospect of improvement,
must have informed the patient about their own situation and prognosis, - must have concluded, together with the patient, that there is no reasonable alternative in the specific situation,
- must have consulted at least one other independent doctor who has seen the patient in person and assessed in writing whether the aforementioned due diligence criteria have been met,
- must have acted with the requisite medical care and attention when terminating life or assisting in suicide.
Similar criteria apply in many other countries.
“The Dutch system is consistently geared towards the due diligence criteria,” explained Yvette Schuijt, a lawyer at the Nederlandse Vereniging voor een Vrijwillig Levenseinde (NVVE), to Medscape.
The primary aim of the legislation is to provide legal protection for doctors and to ensure that, provided the guidelines are followed, no criminal prosecution for homicide offences takes place.
However, the legislation was not designed as a medical protocol to optimise the biological or physiological quality of the dying process.
“There is a significant lack of clinical research into medicines at the end of life.
The specific pharmacodynamic and pharmacokinetic effects are rarely systematically investigated or critically examined in the country,” said Schuijt.
Consequently, potential side effects are not systematically recorded, as they are not subject to regulatory scrutiny. “We assume the procedure works because the patient dies,” said Keizer.
“However, further questions regarding the biological processes are not part of the standard assessment.”
A look at complications
Known complications of the intravenous method include problems with venous access and extravasations, which cause pain and can prevent the patient from reaching a deep coma.
Furthermore, patient-specific physiological factors can impair the onset of action. In the case of a patient treated by Göbel, the blood was so viscous that the administered substances spread only slowly beyond the injection site.
In other cases, the veins are at risk of collapsing due to structural fragility. Oral administration is associated with other risks, including vomiting or the inability to fully ingest the lethal 100 ml solution within a sufficiently short period of time.
Although these complications are considered rare, it is reasonable to assume that they are significantly underreported internationally.
A report from Oregon dating from 2023 shows that in 72% of cases, no information on complications was available.
In the available data sets, adverse events occurred in 9.8% of patients, including difficulties in ingestion, regurgitation and seizures.
In Western Australia, a total of 18 complications were documented in 451 medically assisted deaths between 2024 and 2025.
These predominantly involved problems with intravenous access, regurgitation and seizures.
Other reported events included coughing, delayed loss of consciousness, transient pain and technical difficulties in assembling the syringes.
However, the relevant regulatory authority does not collect data on complications in cases of death by self-administration. Furthermore, neither other Australian states or territories nor New Zealand systematically report on complications.
The Swiss organisation Dignitas and the Federal Ministry of Health declined to provide available data to Medscape.
In Italy, too, no data on complications is collected.
The lack of systematically collected data means that the evidence remains largely anecdotal, according to Pleiter.
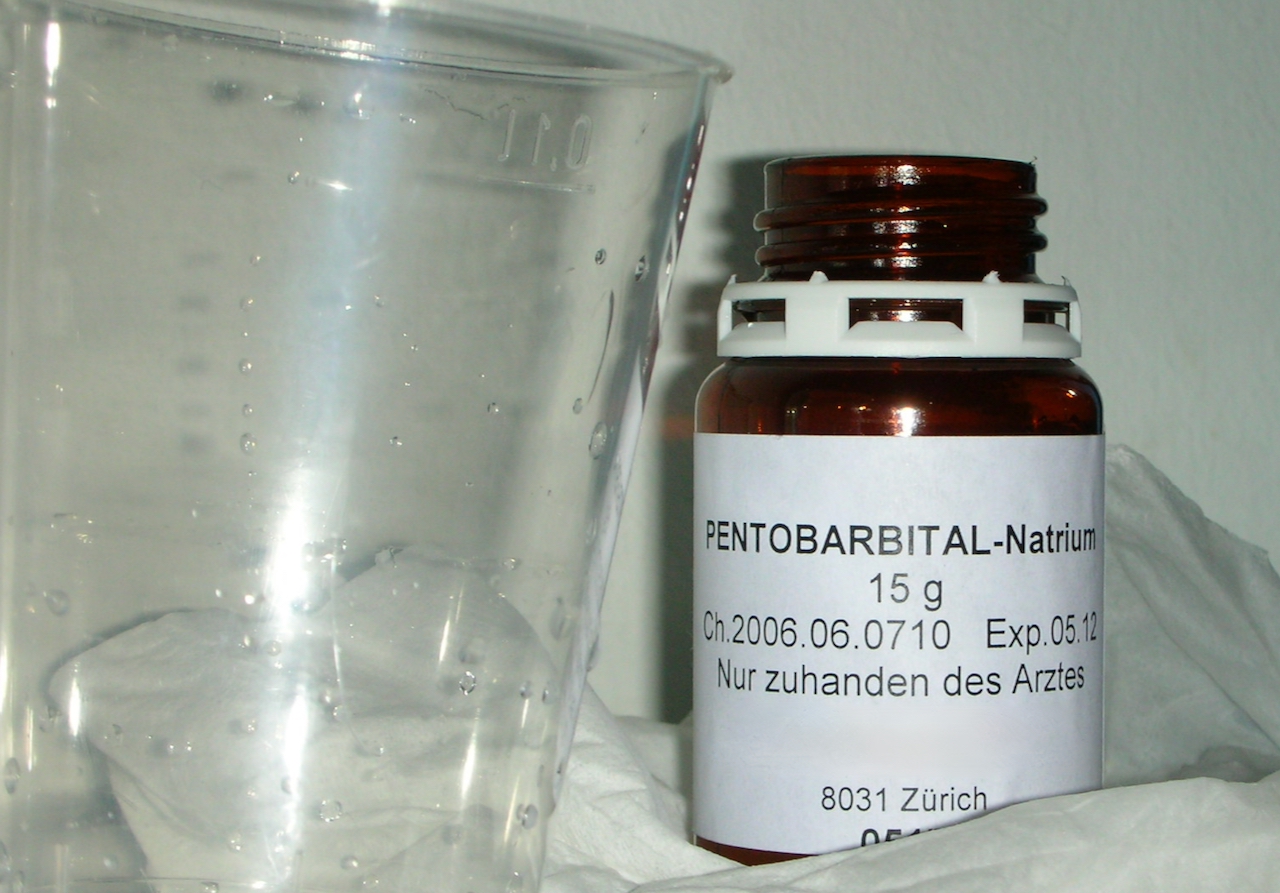
A bottle of Nembutal as used at the Dignitas clinic
The time to death also varies considerably and ranges – depending on the substances used, the route of administration and the patient’s individual physiology – from a few minutes to several hours.
This variability can be distressing for both those affected and their relatives, particularly when a swift and peaceful death is expected, Claud Regnard, a former palliative care physician in the United Kingdom, told Medscape.
Peter Warren, director of the Barcelona-based World Federation of Right to Die Societies, wrote to Medscape that whilst the drugs used in euthanasia and assisted dying differ from country to country, their efficacy and safety have not been studied comparatively.
“To my knowledge, no such consolidated data exists.”
The physiology of death
What happens in the body when euthanasia drugs are administered? Dr Philippe Camus, Professor of Pneumology and Internal Intensive Care Medicine at Dijon University Hospital, has been studying the effects of drugs on the lungs since 1972.
He began systematically collecting data whilst still a medical student at the University of Burgundy. Over more than five decades, he has built up a global database containing over 200,000 references on drug-induced lung diseases.
Even at therapeutic doses, Camus notes, anaesthetics such as propofol can cause respiratory depression, a deep coma, peripheral vasodilation and myocardial dysfunction.
When used as intended, however, these effects are generally mild and easily managed. “The poison is in the dose,” says Camus.
Under the Dutch intravenous euthanasia protocol, the patient receives 1,000 mg of propofol.
A typical dosage for induction of anaesthesia during surgical procedures is 2–2.5 mg/kg body weight intravenously, administered at a rate of approximately 40 mg every 10 seconds.
So far, it has not yet been fully understood how a very high dose of an anaesthetic leads to death, said Didier Cataldo, a pulmonologist at the University of Liège in Liège.
The substances shut down the central respiratory drive in the brain.
The patient falls into a coma, breathing slows down and becomes shallow. A deep coma can lead to the loss of the airway’s protective reflexes, so that the cough and gag reflexes fail to occur.
The tongue falls back, obstructing the upper airways and making it difficult to breathe in. This creates negative pressure in the chest.
When the diaphragm contracts to draw air into the lungs against a closed glottis, the pressure in the alveoli drops rapidly and falls significantly below the pressure in the surrounding blood vessels.
This pressure gradient acts like a suction pump: fluid – and sometimes red blood cells – is drawn from the pulmonary capillaries through the thin membrane into the alveoli. This results in negative pressure pulmonary oedema.
For this reason, patients undergoing surgical procedures are often intubated and ventilated before the full dose of anaesthetic is administered.
In addition, anaesthetics can cause vasodilation and myocardial dysfunction, leading to an abrupt drop in blood pressure and severely impairing cardiac ejection fraction.
Indications of pulmonary oedema
Cataldo pointed out that whilst pulmonary oedema is not classically associated with barbiturate overdoses, its actual prevalence has never been systematically recorded.
Rare physical evidence of this mechanism is provided by a case report from Japan published last year in the Journal of Emergencies, Trauma, and Shock.
In it, doctors describe the death of an 18-year-old man following a lethal overdose of pentobarbital – the same barbiturate used in assisted dying by oral administration.
By the time the emergency services arrived, the patient was already in cardiac arrest. However, according to the publication, a “significant amount of frothy, bloody secretions” emerged from the throat during intubation.
A post-mortem CT scan confirmed severe bilateral pulmonary oedema. The lungs were heavily infiltrated with fluid. The patient, sedated but possibly not yet dead, may have attempted to breathe against an obstructed airway and, in a sense, suffocated from within.
Cataldo explained that such pulmonary oedema can indeed result from breathing efforts against a blocked airway.
Alternatively, severe hypoxia can lead to increased vascular permeability: The capillary walls lose their integrity, become permeable, and fluid passes from the vascular system into the alveoli.
There it forms a foamy barrier that blocks gas exchange. It is plausible that this mechanism – if it occurs – is associated with the terminal stages of agony, according to Cataldo.
Another possible mechanism of death in euthanasia is cardiac-induced pulmonary oedema, explained Bernard Lambermont, Head of the Intensive Care Unit at the University Hospital of Liège.
In this scenario, the heart continues to beat initially, whilst lung function has already failed.
In particular, the left side of the heart, which supplies the systemic circulation, decompensates early or acutely.
The blood remaining in the pulmonary circulation backs up, and the pressure in the fine pulmonary capillaries rises abruptly.
The vessel walls cannot withstand this pressure, become permeable, and fluid leaks out.
Mixed with the remaining air in the lungs, this forms a foam that blocks oxygen exchange.
Camus described the experience of pulmonary oedema as ‘drowning on dry land’.
It is akin to trying to breathe through an extremely narrow straw.
Each breath does not draw in air, but a mixture of blood and fluid that is whipped into a thick, pink foam.
This rises up the trachea and obstructs the airways. The hypoxic brain reacts with a state of panic.
Göbel, who has performed dozens of euthanasia procedures during his career, emphasised, however, that he was “very certain” that patients would not experience pulmonary oedema as conscious suffering.
Opponents of the British draft bill on assisted dying demonstrate with placards outside Parliament in London whilst the House of Lords debates the bill (19 September 2025).
“Propofol completely shuts down cortical consciousness and puts the patient into a deep coma,” said Federico Piffer, a specialist and consultant in pulmonology at the pulmonology department of Arco Hospital in Trento, Italy.
“Even if the body suffers a physiological trauma such as pulmonary oedema, the patient is so deeply anaesthetised that they perceive neither a sensation of drowning nor shortness of breath. In effect, they die under the same complete lack of sensation as would be expected during major surgical procedures.”
Lambermont agreed that such a high dose of an anaesthetic ensures that the patient is deeply anaesthetised when respiratory or cardiac depression occurs.
According to Göbel, the patient first falls into a deep coma; only afterwards does breathing cease. And only once complete unconsciousness has set in is the muscle relaxant administered – 150 mg of rocuronium.
Göbel adds that, in his experience, 9 out of 10 patients have already died by the time they receive the injection of the muscle blocker, which alleviates concerns that someone might be paralysed but still conscious and in pain.
“Once the drug reaches where it’s supposed to work, the process is very predictable. That’s the beauty of it,” he said. “I’ve never seen anyone suffer from it; on the contrary, quite the opposite.
You hold the hands of your children, your loved ones, and whilst you are talking, you gradually become drowsy and lose consciousness within about 20, 30 or 40 seconds.”
Lessons from organ donation
Some reassurance might come from the examination of organs removed following euthanasia. In the Netherlands, Belgium and Canada, patients undergoing euthanasia can opt for organ donation.
Stephen Potts, a transplant psychiatrist at the Royal Infirmary of Edinburgh in Edinburgh, Scotland, explained that organs – including lungs – removed immediately after euthanasia had shown “good clinical outcomes” in recipients.
“It is fair to say that there are many uncertainties regarding the potential toxic effects of these drugs, but these uncertainties are largely theoretical and have not yet manifested in practice.”
Frank Dor, a transplant surgeon at Erasmus MC in Rotterdam, the Netherlands, told Medscape that he had not observed any organ damage.
“The quality of the organs is generally excellent. In fact, they are often better than organs from donors following cardiopulmonary arrest,” said Dor.
Recent data from a systematic review suggest that organ donations following euthanasia achieve comparable outcomes to donations following circulatory death, particularly in lung and kidney transplants.
However, the data on organ transplantation following euthanasia is limited. What is available so far comes from highly controlled clinical settings.
The suitability of the organs for transplantation might suggest that a ‘good death’ is physiologically possible, but whether euthanasia actually represents a pain-free end remains a secret that is buried with the patients as long as no systematic data is collected.
“We lack public data describing how the end of life unfolds and allowing for a clinical assessment of why and how it happens,” said Camus.
Medicine bears responsibility
For Sandra Andoulsi, a 31-year-old dancer and artist from Paris, France, living with Ehlers-Danlos syndrome means waking up every morning with a body that feels as though it is falling apart.
When the pain is unbearable, the abstract risk of a difficult death is irrelevant compared to the concrete torment of her daily existence, said Andoulsi, who is considering euthanasia. “When you’re drowning,” she said, “you don’t ask whether the lifebuoy is made of certified rubber. You just grab hold of it.”
Sandra Andoulsi, a 31-year-old dancer and artist from Paris, lives with Ehlers-Danlos syndrome and is considering euthanasia.
For someone experiencing unbearable suffering, uncertainties regarding the process of dying are acceptable as long as it brings the longed-for relief, said Iline Ceelen, a PhD student at Radboud University in Nijmegen, the Netherlands, to Medscape.
He recalls a patient she interviewed as part of her research, whose arms were covered in scars from self-harm – burns and cuts she had inflicted on herself to cope with her inner torment.
For a woman who was already living in hell, Ceelen said, the prospect of 10 minutes of possible distress during the procedure was a small price to pay for the certainty of an end.
“If someone had told her, ‘It might be hell for 10 minutes’, she wouldn’t have replied, ‘Oh no, no, I’d rather not do it then.’”
Yet Andoulsi is not prepared to absolve the medical system of responsibility so easily.
Whilst she admits she would endure “10 minutes of hell” if it guaranteed an end to her suffering, she finds it unreasonable to be faced with this choice at all.
For Andoulsi, it is a matter of a final act of trust in a system that has repeatedly let her down.
“I’ve spent years fighting against doctors who didn’t believe my pain, who manipulated me and convinced me that it was all in my head,” she said.
“Now that they finally want to help me die, the absolute minimum I expect is that they have done their homework. After a life full of medical negligence, I shouldn’t have to worry that my death will also be negligent.”
Exit